KNOWLEDGE AND ATTITUDES TOWARD ANAPHYLAXIS PREVENTION AND MANAGEMENT OF NURSES, MIDWIVES, AND TECHNICIANS AT VINMEC SMART CITY HOSPITAL IN 2025
ABSTRACT
Objective: (i) To describe the level of knowledge and attitudes regarding anaphylaxis prevention and management among nurses, midwives, and medical technicians at Vinmec Smart City Hospital in 2025. (ii) To identify factors associated with knowledge and attitudes toward anaphylaxis prevention and management among the study participants.
Methods: A descriptive cross-sectional study was conducted among 109 healthcare professionals (nurses, midwives, and medical technicians) working at Vinmec Smart City Hospital in 2025. Data was collected using a structured, self-administered questionnaire that assessed demographic characteristics, knowledge of anaphylaxis recognition and management, and attitudes toward anaphylaxis prevention and response. Descriptive statistics were used to summarize participants’ characteristics and outcome measures. Inferential statistical analyses were performed to identify factors associated with knowledge and attitude levels. A p-value of <0.05 was considered statistically significant.
Results: A total of 109 healthcare professionals participated in the study, including nurses, midwives, and medical technicians working at Vinmec Smart City Hospital. The mean overall knowledge score on anaphylaxis prevention and management was 26.7 ± 3.4 out of 37, and only 26.6% of participants achieved the required knowledge level (≥80%). Among knowledge domains, management knowledge showed the highest pass rate (62.4%), whereas knowledge of clinical scenarios was markedly limited, with a pass rate of only 4.6%.
Regarding attitudes, 67.0% of participants met the required attitude threshold toward anaphylaxis prevention and management. Participation in training related to Circular 51/2017/TT-BYT, both within and outside the Vinmec system, was significantly associated with differences in knowledge levels (p < 0.05). In contrast, positive attitudes were significantly associated with postgraduate qualifications (OR = 8.3; 95% CI: 1.05–65.9; p = 0.019).
Conclusion: Although healthcare professionals at Vinmec Smart City Hospital showed generally acceptable knowledge and positive attitudes toward anaphylaxis prevention and management, important knowledge gaps remain. Regular refresher training standardized clinical guidelines, and simulation-based education are recommended to enhance competency and ensure safe, effective management of anaphylaxis in clinical practice.
Keywords: Anaphylaxis; knowledge; attitude; nurses; midwives; patient safety technicians, Vinmec Smart City Hospital, Vietnam.
Anaphylaxis is a severe, systemic hypersensitivity reaction characterized by a rapid onset and the potential for fatal outcomes if not diagnosed and treated promptly. As a critical medical emergency, it demands immediate clinical recognition and decisive intervention; intramuscular adrenaline remains the first-line and mandatory treatment [3, 4]. Globally, the incidence of anaphylaxis has been rising over the past decades. In the United States, national data show that hospitalizations related to anaphylaxis approximately doubled between 1999 and 2009 [7, 11, 12]. Similarly, a systematic review in Europe indicates that the incidence ranges from 1.5 to 7.9 per 100,000 person-years, with a sustained upward trend [11].
In Vietnam, anaphylaxis is frequently encountered in clinical practice, commonly triggered by medications, food, chemicals, and vaccines. To address this, the Ministry of Health issued Circular 51/2017/TT-BYT, which provides comprehensive guidelines for the prevention, diagnosis, and management of anaphylaxis. This directive aims to standardize clinical protocols and enhance patient safety nationwide [8]. Despite these efforts, the practical application of and adherence to these guidelines continue to face significant challenges and limitations.
Numerous studies demonstrate that the knowledge and attitudes of healthcare professionals are critical to the successful identification and management of anaphylaxis. Cardona et al. [3] emphasize that delays in adrenaline administration often result from a lack of clinical knowledge or hesitation among medical staff. This gap is further highlighted by González-Díaz et al. [5], whose survey in Mexico found that while a majority of healthcare workers identified adrenaline as the first-line treatment, the rate of correct responses regarding the precise dosage and route of administration remained low. Similarly, research in Saudi Arabia indicated that only approximately 40% of healthcare providers possessed adequate knowledge of anaphylaxis management, though the study noted that simulation-based training significantly enhanced clinical practice [1].
In Vietnam, preliminary research reflects similar challenges regarding clinical preparedness. A study by Nguyen Hai Lam demonstrated that only approximately 30% of nurses possessed satisfactory knowledge concerning the management of anaphylaxis [9]. Furthermore, research conducted by Ta Thi Anh Tho at K Hospital highlighted significant limitations in nurses' ability to recognize symptoms and execute correct adrenaline injection protocols [14]. These findings suggest that, beyond core professional competency, a proactive attitude toward updating knowledge and strictly adhering to clinical guidelines is a critical factor in determining the quality of emergency management [2, 10].
Moreover, the literature indicates that health workers’ knowledge and attitudes toward anaphylaxis are shaped by multiple individual and professional factors, including gender, educational attainment, clinical specialty, years of experience, and participation in relevant training programs [6, 10]. In particular, simulation-based education has increasingly been shown to enhance practical competence and facilitate the transfer of knowledge to real-world emergency decision-making and skills performance [1, 6].
Vinmec Smart City Hospital operates under an international hospital model in Vietnam, where healthcare professionals routinely care for patient groups at heightened risk of anaphylaxis. Assessing the current knowledge and attitudes of nurses, midwives, and medical technicians at this hospital therefore serves not only as an indicator of workforce readiness but also as an empirical foundation for optimizing training strategies to strengthen anaphylaxis response capacity and improve patient safety.
On this basis, we conducted the study entitled “Knowledge and Attitudes about Anaphylaxis Prevention and Treatment Management of Nurses, Midwives, and Technicians at Vinmec Smart City Hospital in 2025” to describe current knowledge and attitudes, identify associated factors, and inform feasible recommendations for improvement.
II. RESEARCH POPULATION AND METHODS
Study population: The study population consisted of nurses, midwives, and medical technicians working at Vinmec Smart City Hospital in 2025. These healthcare professionals are directly involved in patient care, medication administration, and clinical procedures, including the initial recognition and management of patients at risk of anaphylaxis. Therefore, assessing their knowledge and attitudes has important practical implications for improving emergency response capacity and patient safety.
- Inclusion criteria: were healthcare professionals who had been working at the hospital for at least six months and voluntarily agreed to participate in the study by providing informed consent.
- Exclusion criteria: including staff who were on long-term leave during the data collection period, those who declined participation, or questionnaires with more than 20% missing responses.
Time and setting: The study was conducted at Vinmec Smart City Hospital, Hanoi, Vietnam, from July to September 2025.
Study design: A descriptive cross-sectional study design was employed to assess the current level of knowledge and attitudes regarding anaphylaxis prevention and management among healthcare professionals at a single point in time. In addition, the study examined the associations between sociodemographic and professional characteristics and knowledge and attitude outcomes.
Sample size and sampling method: The sample size was calculated using the formula for estimating a population proportion, with the following parameters: expected proportion (p) = 0.5, confidence level of 95% (Z = 1.96), and margin of error (d) = 0.1. The minimum required sample size was 96 participants. After adjusting for an anticipated non-response rate of 10%, the final minimum sample size was 106.
A total of 109 valid questionnaires were collected, satisfying the required sample size. Participants were selected using a convenience sampling method, whereby all eligible healthcare professionals from clinical departments with a high risk of anaphylaxis as well as selected subclinical departments were invited to participate during the study period.
Study variables
- Dependent variables:
- Knowledge level regarding anaphylaxis prevention and management.
- Attitudes toward anaphylaxis prevention and management.
- Independent variables:
- Sociodemographic characteristics: gender, age, profession, educational level.
- Professional characteristics: department, years of experience in healthcare, duration of employment at Vinmec Smart City Hospital, prior training on anaphylaxis, and exposure to Circular 51/2017/TT-BYT.
Data collection instruments and procedures: Data were collected using a structured, self-administered questionnaire developed based on Circular 51/2017/TT-BYT on the prevention, diagnosis, and management of anaphylaxis, in combination with international guidelines, including the World Allergy Organization Anaphylaxis Guidelines (2020) and the Anaphylaxis Practice Parameter Update (2023), as well as instruments used in previous domestic and international studies.
The questionnaire comprised three sections: (i) Demographic and professional characteristics; (ii) Knowledge assessment, consisting of 37 multiple-choice questions covering causes, recognition, diagnosis, management, prevention, and clinical scenarios of anaphylaxis. Each correct answer was awarded one point, with a maximum score of 37. Knowledge was considered adequate when participants achieved ≥80% of the total score; (iii) Attitude assessment, consisting of 21 items measured on a five-point Likert scale, with a maximum total score of 105. Attitudes were classified as positive when participants achieved ≥80% of the total score. The questionnaire was pilot tested on a small group of healthcare professionals to assess clarity, feasibility, and internal consistency prior to official data collection.
Data collection procedures: Data were collected through both paper-based questionnaires and electronic surveys. All participants were informed about the study objectives, assured of anonymity and confidentiality, and informed that the collected data would be used solely for research purposes. The average time required to complete the questionnaire was approximately 15–20 minutes. Questionnaires with incomplete responses exceeding 20% of the total items were excluded from the analysis.
Data analysis: Data was entered and analyzed using SPSS version 20.0. Descriptive statistics, including frequencies, percentages, means, and standard deviations, were used to summarize participant characteristics and study variables. Associations between independent variables and knowledge or attitude levels were examined using Chi-square tests. Odds ratios (ORs) with 95% confidence intervals (CIs) were calculated to quantify the strength of associations. Statistical significance was set at p < 0.05.
Ethical considerations
The study was approved by the Ethics Committee in Biomedical Research of Vinmec Smart City Hospital. All participants were fully informed about the study objectives, procedures, rights, and obligations prior to participation. Written informed consent was obtained from all participants. Confidentiality of personal information was strictly maintained, and participants were free to withdraw from the study at any time without any impact on their professional rights or interests.
3.1. Characteristics of the research object
Table 3.1: General information of the research subjects (n=109)
|
General characteristics |
Quantity (N) |
Rate (%) |
|
|
Departmental |
Clinicaldepts(highriskofanaphylaxis) |
82 |
75,2 |
|
Subclinical depts (lower risk of anaphylaxis) |
27 |
24,8 |
|
|
Gender |
Male |
18 |
16,5 |
|
Female |
91 |
83,5 |
|
|
Education |
Colleges and universities |
94 |
86,2 |
|
Postgraduate |
15 |
13,8 |
|
|
Training Expertise |
Nursing |
86 |
78,9 |
|
Midwifery, Technician |
23 |
21,1 |
|
|
Working time at Vinmec |
< 3 years |
57 |
52,3 |
|
≥ 3 years |
52 |
47,7 |
|
|
Total years of experience in the medical profession |
< 5 years |
46 |
42,2 |
|
≥ 5 years |
63 |
57,8 |
|
|
Participated in training on prevention and management of anaphylaxis at Vinmec |
Trained |
51 |
46,8 |
|
Untrained/unremembered |
58 |
53,2 |
|
|
Participated in training on prevention and management of anaphylaxis outside the Vinmec system |
Trained |
46 |
42,2 |
|
Untrained/unremembered |
63 |
57,8 |
|
|
Total |
109 |
100 |
|
Comments:
Among the 109 participants, most were female (83.5%) and worked in clinical departments with a high risk of anaphylaxis (75.2%). The majority were nurses (78.9%) and held a college or university degree (86.2%). More than half had worked at Vinmec for less than three years, while over half reported at least five years of total professional experience. Fewer than half had received training on anaphylaxis prevention and management either within or outside the Vinmec system.
3.2. Knowledge and attitude about anaphylaxis prevention and management
Table 3.2: Knowledge scores for anaphylaxis prevention and management (n=109)
|
Knowledge of anaphylaxis prevention and management |
Mean |
SD |
Min |
Max |
|
Knowledge of causes and mechanisms (7 items: A.1 – A.7) |
4,9 |
1,5 |
1 |
7 |
|
Knowledge of anaphylaxis diagnosis (4 items: B.1 – B.4) |
2,8 |
0,9 |
1 |
4 |
|
Knowledge of management (16 items: C.1 – C.16) |
12,8 |
1,8 |
8 |
16 |
|
Knowledge of contingency (6 items: D.1 – D.6) |
3,9 |
1,1 |
1 |
6 |
|
Knowledge of assessment situation (4 items: F.1 – F.4) |
2,3 |
0,8 |
1 |
4 |
|
General Knowledge (37 items: A1 – F4) |
26,7 |
3,4 |
19 |
34 |
Comments:
The mean overall knowledge score was 26.7 ± 3.4 out of 37 points. Management-related knowledge had the highest mean score, whereas situational assessment knowledge showed the lowest mean score among all domains.
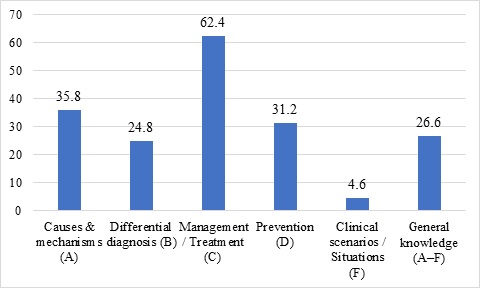
Figure 3.1. Proportion of participants achieving adequate knowledge of anaphylaxis prevention and management by knowledge domain (n = 109)
Comments: Figure 3.1 illustrates the proportion of participants achieving adequate knowledge of anaphylaxis prevention and management across different knowledge domains. The highest proportion of participants meeting the adequacy threshold was observed in the management domain, whereas the lowest proportion was found in the clinical scenario and contingency domain. The remaining domains showed intermediate levels of adequate knowledge.
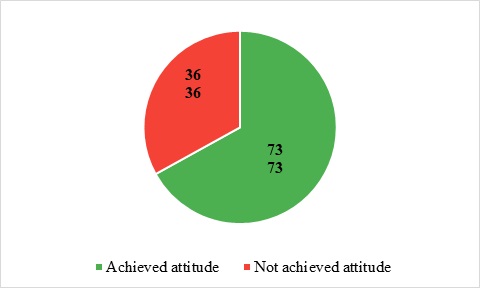
Figure 3.2. Proportion of participants achieving the required attitude toward anaphylaxis prevention and management (n = 109)
Comments: Figure 3.2 indicates that 73/109 participants (67.0%) achieved the required attitude standard regarding anaphylaxis prevention and management, whereas 36/109 (33.0%) did not.
3.3. Associations between demographic characteristics, knowledge and attitudes toward anaphylaxis prevention and management
Table 3.3: Associations between participant characteristics and knowledge of anaphylaxis prevention and management
|
Associated factors |
Knowledge |
OR (95%CI) |
p |
|
|
Adequate (N/%) |
Inadequate (N/%) |
|||
|
Faculties/Departments |
||||
|
Clinical |
20 (24,4) |
62 (75,6) |
0,6 (0,3 – 1,7) |
0,362 |
|
Subclinical |
9 (33,3) |
18 (66,7) |
||
|
Gender |
||||
|
Male |
4 (22,2) |
14 (77,8) |
0,8 (0,2 – 2,5) |
0,645 |
|
Female |
25 (27,5) |
66 (72,5) |
||
|
Education |
||||
|
Colleges and universities |
27 (28,7) |
67 (71,3) |
2,6 (0,6 – 12,4) |
0,35 |
|
Postgraduate |
2 (13,3) |
13 (86,7) |
||
|
Training Expertise |
||||
|
Nursing |
25 (29,1) |
61 (70,9) |
1,9 (0,6 – 6,3) |
0,302 |
|
Midwifery, Technician |
4 (17,4) |
19 (82,6) |
||
|
Working time at Vinmec |
||||
|
< 3 years |
12 (21,1) |
45 (78,9) |
0,5 (0,2 – 1,3) |
0,17 |
|
≥ 3 years |
17 (32,7) |
35 (67,3) |
||
|
Total length of professional clinical experience |
||||
|
< 5 years |
11 (23,9) |
35 (76,1) |
0,8 (0,3 – 1,9) |
0,6 |
|
≥ 5 years |
18 (28,6) |
45 (71,4) |
||
|
Participated in training on anaphylaxis prevention and management of within Vinmec system |
||||
|
Untrained/unknown |
22 (37,9) |
36 (62,1) |
3,8 (1,5 – 10,01) |
0,004 |
|
Trained |
7 (13,7) |
44 (86,3) |
||
|
Participated in training on anaphylaxis prevention and management outside Vinmec system |
||||
|
Untrained/unknown |
23 (36,5) |
40 (63,5) |
3,8 (1,4 – 10,4) |
0,006 |
|
Trained |
6 (13) |
40 (87) |
||
Comments:
Analysis of Table 3.3 shows that most sociodemographic and professional characteristics—including department, gender, educational level, professional specialty, duration of employment at Vinmec, and total clinical experience, were not significantly associated with adequate knowledge of anaphylaxis prevention and management (p > 0.05). In contrast, participation in anaphylaxis-related training was significantly associated with knowledge levels. Participants who had not attended or were unaware of training within the Vinmec system were more likely to have adequate knowledge compared with those who had received training (OR = 3.8; 95% CI: 1.5–10.01; p = 0.004). A similar association was observed for training participation outside the Vinmec system (OR = 3.8; 95% CI: 1.4–10.4; p = 0.006).
Table 3.4: Association between participant characteristics and attitudes toward anaphylaxis prevention and management
|
Associated factors |
Attitude |
OR (95%CI) |
p |
|
|
Adequate / (N/%) |
Inadequate (N/%) |
|||
|
Faculties/Departments |
||||
|
Clinical |
59 (72) |
23 (28) |
2,4 (0,97 – 5,8) |
0,054 |
|
Subclinical |
14 (51,9) |
13 (48,1) |
||
|
Gender |
||||
|
Male |
10 (55,6) |
8 (44,4) |
0,6 (0,2 – 1,6) |
0,26 |
|
Female |
63 (69,2) |
28 (30,8) |
||
|
Education |
||||
|
Postgraduate |
14 (93,3) |
1 (6,7) |
8,3 (1,05 – 65,9) |
0,019 |
|
Colleges and universities |
59 (62,8) |
35 (37,2) |
||
|
Training Expertise |
||||
|
Nursing |
59 (68,6) |
27 (31,4) |
1,4 (0,5 – 3,6) |
0,484 |
|
Midwifery, Technician |
14 (60,9) |
9 (39,1) |
||
|
Working time at Vinmec |
||||
|
< 3 years |
38 (66,7) |
19 (33,3) |
0,97 (0,4 – 2,2) |
0,094 |
|
≥ 3 years |
35 (67,3) |
17 (32,7) |
||
|
Total length of professional clinical experience |
||||
|
< 5 years |
30 (65,2) |
16 (34,8) |
0,9 (0,4 – 1,95) |
0,739 |
|
≥ 5 years |
43 (68,3) |
20 (31,7) |
||
|
Participated in training on prevention and management of anaphylaxis at Vinmec |
||||
|
Trained |
37 (72,5) |
14 (27,5) |
1,6 (0,7 – 3,6) |
0,246 |
|
Untrained/unknown |
36 (62,1) |
22 (37,9) |
||
|
Participated in training on prevention and management of anaphylaxis outside Vinmec |
||||
|
Trained |
33 (71,7) |
13 (28,3) |
1,5 (0,6 – 3,3) |
0,366 |
|
Untrained/unknown |
40 (63,5) |
23 (36,5) |
||
Comment: Most unrelated factors make sense for attitude (p > 0.05). However, the group with a postgraduate degree had a markedly higher achievement attitude than the college/university group (93.3% vs. 62.8%), OR = 8.3 (95% CI: 1.05–65.9; p = 0.019).
IV. DISCUSSION
4.1. Characteristics of the study population
The results indicate that the majority of participants were female (83.5%), held a college or university degree (86.2%), and belonged to the nursing profession (78.9%). This distribution reflects the the structure of the healthcare workforce in Vietnam, where nurses—predominantly women—play a central role in direct patient care. More than half of the participants had worked at Vinmec for less than three years (52.3%), and 42.2% reported fewer than five years of total professional experience, suggesting a relatively young workforce that may have limited clinical exposure to the recognition and management of anaphylaxis. This finding is consistent with several international studies highlighting practical experience as a key determinant of competence in anaphylaxis identification and treatment [3, 5, 6].
Notably, only 46.8% of participants had received training on Circular 51/2017/TT-BYT within Vinmec system and 42.2% had undergone such training outside the system.Theseproportion underscore the need to strengthen regular training programs and implement post-training competency assessments, in line with the recommendations from international guidelines such as WAO 2020 and AAAAI 2023 [3].
4.2. Knowledge and attitude toward anaphylaxis prevention and management
The participants’ mean overall knowledge score was 26.7 ± 3.4 out of 37, and only 26.6% met the predefined adequacy threshold (≥80%). Among the knowledge domains, management knowledge yielded the highest mean score (12.8/16); however, when classified using the adequacy criterion, only 62.4% achieved the required level. Most notably, the pass rate for clinical scenario/contingency knowledge was only 4.6%, indicating substantial limitations in translating theoretical knowledge into practical decision-making and response in real-life anaphylaxis situations.
These findings are consistent with prior evidence. Şimşek et al. reported that, despite awareness of the correct first-line medication, pediatric nurses demonstrated very low competence in adrenaline management in real-world contexts [13]. Similarly, a Vietnamese study by Nguyen Hai Lam found that only about 30% of nurses had adequate knowledge of anaphylaxis management, with particularly weak performance in scenario recognition and application [9]. Collectively, the results suggest that gaps in practical, situation-based anaphylaxis knowledge remain common, even within an international hospital setting.
In contrast to the knowledge findings, the proportion of participants meeting the required attitude standard was relatively high (67%). Most respondents agreed that anaphylaxis is a medical emergency requiring rapid management in accordance with established protocols, reflecting a strong sense of professional responsibility in patient care. However, the coexistence of favorable attitudes and limited knowledge suggests a persistent gap between awareness and practical competence—an issue consistently reported in the international literature [1, 5, 13].
Oluwole et al. reported that higher educational attainmentis associated with more positive professional attitudes and greater receptiveness to clinical guidance and training [10]. Consistent with this evidence, the present study found a substantially higher rate of adequate attitudes among participants with postgraduate qualifications compared with those without (93.3% vs. 62.8%). This pattern suggests that advanced education may strengthen risk perception and reinforce the perceived importance of strict adherence to anaphylaxis management protocols.
4.3. Factors affecting knowledge and attitudes about anaphylaxis prevention and management
In the association analysis, most of demographic and occupational characteristics were not significantly associated withwith knowledge or attitude outcomes. Notably, participation in Circular 51/2017/TT-BYT training showed an unexpected inverse association with knowledge: participants who reported never having attended—or not knowing about—such training demonstrated a higher knowledge pass rate than those who had attended training (p < 0.05). This counterintuitive pattern may indicate limitations in the current training approach, which may be overly didactic and insufficiently focused on scenario-based practice and simulation—elements consistently shown to be critical for strengthening anaphylaxis management competence [1, 2, 6].
Regarding attitudes, postgraduate qualification was the only factor significantly associated with meeting the required attitude standard (OR = 8.3), suggesting that advanced education may enhance professional readiness and reinforce the perceived importance of protocol adherence. In contrast, gender, department, and working duration were not associated with attitude differences. This is consistent with Krugman’s systematic evidence indicating that education and accumulated clinical experience are key determinants of preparedness, whereas gender or baseline professional grouping contributes minimally to attitudinal variation [6].
4.4. Study implications
The findings have important practical implications for strengthening anaphylaxis preparedness in clinical settings. First, periodic training should be reinforced and redesigned to prioritize simulation-based learning and scenario-driven drills rather than relying predominantly on didactic instruction. Evidence from international studies indicates that simulation training can substantially improve clinical decision-making, teamwork, and technical performance in emergency management, including anaphylaxis response [2, 6]. Second, post-training monitoring and competency assessment should be institutionalized to evaluate skill retention and to support the sustained maintenance of adequate knowledge and constructive professional attitudes over time. Third, embedding standardized anaphylaxis training into Vinmec’s onboarding and early-career development programs would help address gaps among staff with limited clinical experience and promote consistency of practice across departments.
Overall, this study provides empirical evidence to inform the design and refinement of anaphylaxis training programs in Vietnam and underscores the synergistic value of integrating structured education, experiential learning, and professional attitudes to enhance emergency response capacity.
V. CONCLUSIONS AND RECOMMENDATIONS
This study found that while most nurses, midwives, and technicians at Vinmec reported positive attitudes toward anaphylaxis prevention and management (67%), overall knowledge remained limited, with only 26.6% reaching a satisfactory level. Notably, knowledge related to clinical scenarios and practical application was very low, indicating a substantial gap between awareness and real-world response capacity. Demographic factors such as gender, department, and length of employment were not significantly associated with outcomes; in contrast, higher educational attainment and prior training were more influential.
These findings highlight the need to strengthen and redesign anaphylaxis training programs by prioritizing simulation-based, case-oriented learning and hands-on practice of adrenaline administration, complemented by periodic refresher sessions and post-training competency assessments to ensure retention. Integrating anaphylaxis content into onboarding programs for new staff is also essential to reduce knowledge gaps among those with limited clinical experience. Hospitals should implement routine monitoring and supportive policies that encourage training participation to improve clinical readiness and patient safety. Further multi-center studies are recommended to evaluate the long-term effectiveness of different training models and inform national training and quality-management strategies.
REFERENCES
2. ASCIA (2021), Acute Management of Anaphylaxis. Australia: ASCIA; 2021–2024.
Nguyen Thi Lien1, Nguyen Ngoc Anh1, Phan Thi Thu Hien1, Phan Dinh Huy1, Nguyen Thi Khuyen1, Nguyen Thi Khanh Van1, Pham Nhat Quang1, Pham Van Thanh1, Tran Thi Thu2, Nguyen Phuc Phong2
1. Vinmec Smart City Hospital; 2. Vinmec Times City Hospital
Correspondence author: Nguyen Thi Lien, Email: v.liennt1@vinmec.com; ĐT: 0932356639
Tin mới
-
Thứ trưởng Bộ Y tế, GS.TS Trần Văn Thuấn vừa phê duyệt Đề án Bệnh viện vệ tinh...29/04/2026 15:28
-
Thương hiệu cu đơ Lệ Phương Hà Tĩnh: Khẳng định chất lượng, nâng tầm cạnh tranh
Giữa dòng chảy sôi động của thị trường đặc sản vùng miền, nơi mỗi địa phương đều nỗ...28/04/2026 23:28 -
Bộ Y tế đề xuất mỗi trạm y tế xã có 15 người làm việc, điều chỉnh theo dân số, khu vực
Bộ Y tế đang lấy ý kiến các bộ, ngành, sở y tế địa phương về dự thảo...28/04/2026 10:55 -
Không chủ quan với ngộ độc thực phẩm những ngày nghỉ lễ
Thời tiết nắng nóng cùng với nhu cầu ăn uống, du lịch tăng cao trong dịp nghỉ lễ...28/04/2026 10:22 -
Trung tâm y tế cũ thành khu điều trị mới của Bệnh viện Tai Mũi Họng TP HCM
Trụ sở cũ của Trung tâm Y tế Quận 3 được chuyển đổi thành khu điều trị mới...27/04/2026 11:13 -
Chuyên gia lên tiếng về 'giác hơi hút máu' ở Hà Nội: Sai chuyên môn, đe dọa sức khoẻ, tính mạng
Từ thực tế ghi nhận tại cơ sở không phép ở xã Chương Dương (Hà Nội), theo các...27/04/2026 11:09 -
Rắn độc vào mùa sinh sản, đừng để một phút chủ quan trả giá đắt
Thời gian gần đây, khi bước vào mùa sinh sản của rắn (từ tháng 4 đến tháng 11),...26/04/2026 13:24 -
Phó Bí thư Thường trực Tỉnh ủy Nguyễn Hồng Phong giao lưu bóng bàn, động viên VĐV tại giải thể thao hè Sầm Sơn
Đồng chí Nguyễn Hồng Phong, Ủy viên dự khuyết Trung ương Đảng, Phó Bí thư Thường trực Tỉnh...26/04/2026 13:15 -
Sinh hoạt khoa học điều dưỡng: Nâng cao chất lượng chăm sóc vết thương, hướng tới an toàn người bệnh
Ngày 24/4/2026, Bệnh viện Đa khoa tỉnh Phú Thọ tổ chức buổi sinh hoạt khoa học điều dưỡng...25/04/2026 16:22 -
Ứng dụng công nghệ số, đội ngũ điều dưỡng phát triển bền vững
Trong công cuộc chuyển đổi số của ngành Y tế TP Cần Thơ, đội ngũ điều dưỡng góp...25/04/2026 15:14 -
Bộ Y tế: Không được từ chối, chậm trễ cấp cứu người bệnh dịp nghỉ lễ
Bộ Y tế yêu cầu các đơn vị tổ chức tốt công tác cấp cứu, khám chữa bệnh...25/04/2026 10:24 -
Trao gửi yêu thương – tiếp thêm nghị lực: chương trình tri ân người bệnh nhân ngày quốc tế điều dưỡng 12/5
Điều dưỡng không chỉ là một nghề nghiệp, đó còn là sứ mệnh của sự thấu cảm và...24/04/2026 22:28 -
Lặng thầm nơi “bộ tham mưu nội khoa” của Bệnh viện Trung ương Quân đội 108
Nằm giữa nhịp vận hành khẩn trương của Bệnh viện Trung ương Quân đội 108, Khoa Nội tổng...24/04/2026 14:00 -
Truyền thông, giáo dục sức khỏe – nhiệm vụ quan trọng của điều dưỡng
Trong bối cảnh hiện nay, bên cạnh công tác quản lý và chăm sóc người bệnh cũng như...24/04/2026 14:47